Rhesus Blood Group
ScienceTopping | July 8, 2024
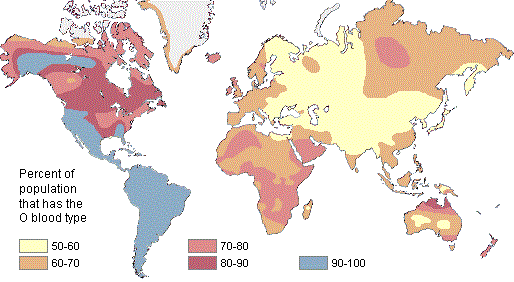 O+ is the most common blood group in the world, accounting for 38% of the world population.
Rhesus blood group is another system developed to classify another types of antigens found on the surface of red blood cells other than the A and B antigens as
in ABO blood group. Rhesus blood group can be deemed as the second most significant blood group just after ABO
blood group due to its alloimmunity reaction triggered especially in specific pregnant women. If ignored or not screened, it can cause serious complications during
pregnancies, namely hemolytic disease of newborn (HDN). Delayed hemolytic transfusion reaction is also another catastrophy brought about by incompactible Rhesus blood group during blood transfusion.
O+ is the most common blood group in the world, accounting for 38% of the world population.
Rhesus blood group is another system developed to classify another types of antigens found on the surface of red blood cells other than the A and B antigens as
in ABO blood group. Rhesus blood group can be deemed as the second most significant blood group just after ABO
blood group due to its alloimmunity reaction triggered especially in specific pregnant women. If ignored or not screened, it can cause serious complications during
pregnancies, namely hemolytic disease of newborn (HDN). Delayed hemolytic transfusion reaction is also another catastrophy brought about by incompactible Rhesus blood group during blood transfusion.
While ABO blood group has A and B antigens, Rhesus blood group has D, C, E, c and e antigens. Among these 5 types of antigens, Rhesus D antigen is the one
manifesting the most severe consequence. When it comes to antigens, there must be antibodies binding to the antigens for an immunogenic reaction to occur. Therefore,
there are anti-D, anti-C, anti-E, anti-c and anti-e antibodies which are mainly IgG antibodies, with IgM antibodies as minority. To date, there are
only a few cases
reporting naturally occurring IgM Rhesus anti-E antibodies which mimick anti-A1 antibodies. Otherwise, as long as Rhesus disease is discussed, anti-D antibodies are
the most notorious culprit accounting for Rhesus disease. Rhesus D antigen is reponsible for 50% of maternal alloimmunisation in pregnancy. In classification of
severity of Rhesus disease, different antibodies produced against Rhesus antigens can cause different severity of Rhesus disease.
- Mild to Moderate: anti-C, anti-E, anti-e
- Severe: anti-D, anti-c
As it has crowned the ranking among all Rhesus antigens in terms of severity and frequency, Rhesus D antigen must be dealt with efficiently in healthcare
infrastructures all around the world. Rhesus antigens are in fact part of a protein complex in red blood cell membrane. The protein complex consists of
2 molecules of Rhesus-associated glycoproteins (RhAG) and 2 molecules of Rhesus proteins.
RhAGs are necessary to direct Rhesus antigens to red blood cell membrane.
If RhAGs are absent, Rhesus antigens will not be present in red blood cell membrane. As for Rhesus proteins, there are 2 types of them, namely RhD and RhCE proteins.
As the names suggest, RhD protein carries Rhesus D antigen, while RhCE protein carries C or c Rhesus antigen along with E or e Rhesus antigens.
The most concerning part of Rhesus factor is Rhesus disease in fetus or newborn. However, there are specific criteria to be fulfilled before Rhesus disease can occur.
Clinical Highlight
Rhesus disease develops in fetus or newborn when
all of the following occur.
- The mother has a Rhesus D (RhD) negative blood group.
- The fetus or newborn has a RhD positive blood group.
- The mother has previously been exposed to RhD positive blood, being sensitised.
If all three criteria are matched,
routine antenatal anti-D prophylaxis (RAADP)
must be given by healthcare professionals to the affected mother at 28 weeks of gestation.
Rhesus factor of a fetus is inherited depending on D or d allele passed from the parents, giving 3 different genotypes, namely DD, Dd and dd genotypes. With D allele
being dominant, both DD and Dd genotypes manifest as RhD positive, while dd genotype manifests as RhD negative.
 D allele is dominant over d allele. Take note that there is no actual d allele present on chromosome 1, being just a
descriptive for the absence of D allele.
It is crucial to comprehend the chronological order of how it occurs. Relevant only in mothers with RhD negative blood group, Rhesus incompactibility
only manifests as Rhesus disease starting from second pregnancy onwards. During one's first pregnancy without any history of miscarriage, if her Rhesus
blood group is RhD negative and the fetus' Rhesus blood group is Rh positive, sensitisation will occur with negligible amount of maternal antibodies produced
against Rhesus antigens of the fetus. However, due to its negligible amount, it is not sufficient yet for Rhesus disease to manifest yet.
D allele is dominant over d allele. Take note that there is no actual d allele present on chromosome 1, being just a
descriptive for the absence of D allele.
It is crucial to comprehend the chronological order of how it occurs. Relevant only in mothers with RhD negative blood group, Rhesus incompactibility
only manifests as Rhesus disease starting from second pregnancy onwards. During one's first pregnancy without any history of miscarriage, if her Rhesus
blood group is RhD negative and the fetus' Rhesus blood group is Rh positive, sensitisation will occur with negligible amount of maternal antibodies produced
against Rhesus antigens of the fetus. However, due to its negligible amount, it is not sufficient yet for Rhesus disease to manifest yet.
Nevertheless,
during the second pregnancy, if the fetus' Rhesus blood group is again RhD positive, previous sensitisation during first pregnancy results in sufficiently large
number of antibodies produced against fetus' Rhesus antigens. Binding between antibodies and Rhesus antigens ultimately cause Rhesus disease. This is the reason
anti-D immunoglobulin must be given at 28 weeks of gestation to prevent HDN.
Rhesus incompatibility is a serious issue, and it may cause fetal loss if no prompt prophylaxis is given by healthcare professionals. Therefore, antenatal care
of pregnant women plays an important role in securing future successful delieveries of babies. Pregnant women must be attending every single follow-up scheduled by
healthcare professionals.
Apart from HDN in pregnancy, it is also important not to forget delayed hemolytic transfusion reaction as a result of Rhesus incompactibility. During blood
transfusion, RhD positive recipient can receive blood from RhD positive or RhD negative donor. Meanwhile, RhD negative recipient can only receive blood from
RhD negative donor, as they cannot tolerate the presence of foreign RhD antigens which are present in RhD positive blood. Hemolysis occurs when antibodies produced
against RhD antigens bind to the antigens, resulting in spontaneous destruction of red blood cells. All in all Rhesus blood group can be deemed to be of similar
level of significance to ABO blood group when it comes to blood screening for blood transfusion as well as during pregnancy.
Clinical Highlight
In case of
emergency blood transfusion
whereby the necessary blood group crossmatch cannot be completed beforehand,
O- blood is used regardless of the recipient's blood group due to its lack of
alloimmunization triggered.
- Blood group O has neither A nor B antigens present on the surface of red blood cell membrane.
- RhD negative blood has no Rhesus D antigens in the red blood cell membrane.
Therefore, every healthcare infrastructure in every country must have sufficient number of O- blood packs reserved for emergency use.